Ultimate Guide to Supply Chain Continuity in Healthcare
Post Summary
Maintaining a steady healthcare supply chain is critical for patient safety. Disruptions can lead to expired products being used or essential items unavailable during procedures, as seen in 57% of cases reported by clinicians. The reliance on third-party vendors and just-in-time models has exposed vulnerabilities, especially during events like the February 2024 Change Healthcare cyberattack, which caused widespread operational failures.
Here’s what you need to know:
- Key Risks: Dependence on single vendors, lack of reliable data, and cybersecurity threats.
- Steps to Improve Continuity:
- Identify critical supply chain functions using tools like Business Impact Analysis (BIA).
- Diversify suppliers to avoid single points of failure.
- Transition to hybrid inventory models (just-in-time + just-in-case).
- Strengthen third-party vendor risk management across vendor networks.
- Technology’s Role: Platforms like Censinet RiskOps™ streamline risk assessments and improve visibility.
- Resilience Requires Action: Regular testing, cross-department collaboration, and updated continuity plans are essential for minimizing disruptions.
Strong leadership, smarter inventory strategies, and secure digital tools are key to ensuring uninterrupted patient care.
The Correlation Between Continuity, Supply Chain Resiliency, and Sustainability in Medical Packaging
sbb-itb-535baee
Healthcare Supply Chain Risks and Vulnerabilities
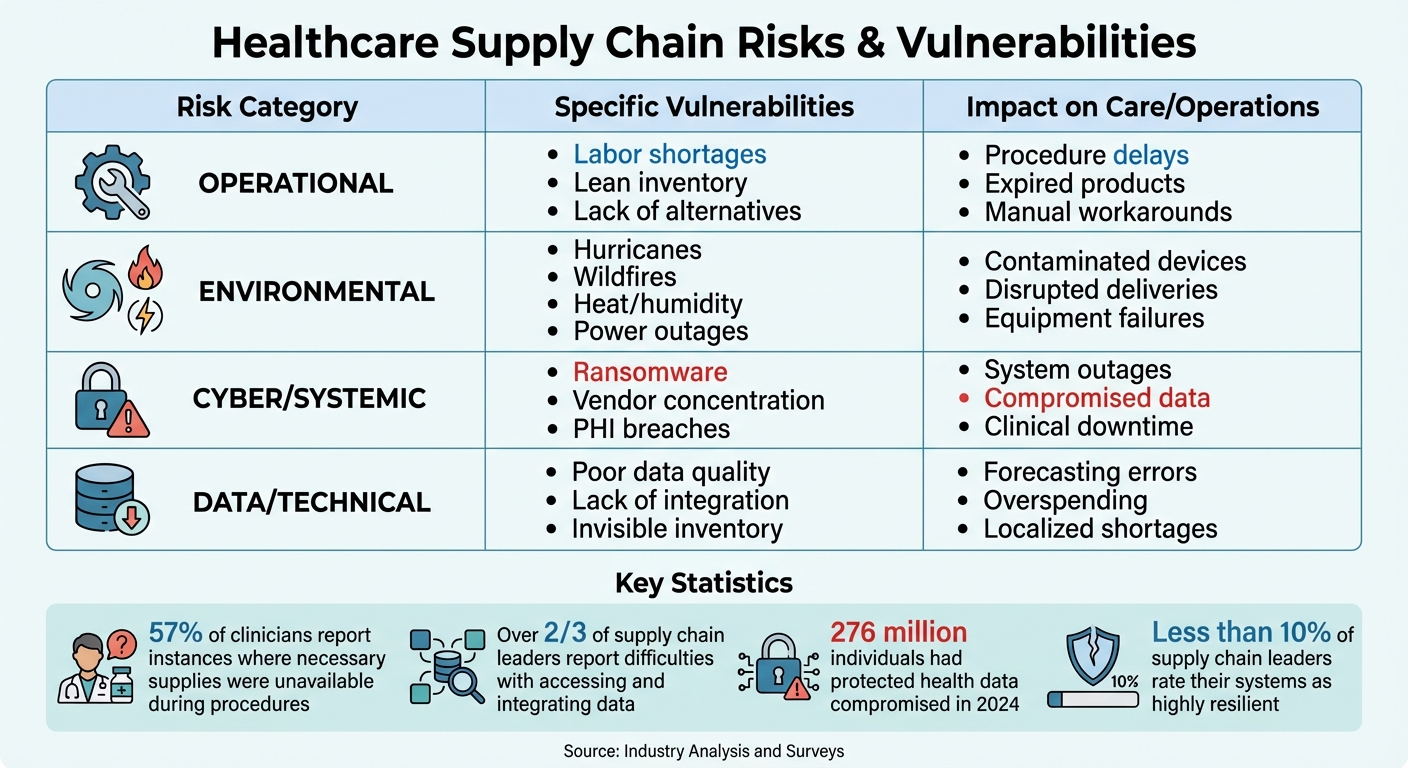
Healthcare Supply Chain Risks: Categories, Vulnerabilities, and Operational Impact
Healthcare supply chains are under immense pressure, facing a mix of risks that can disrupt operations and jeopardize patient safety. The traditional "lean" model, which focuses on cost efficiency through just-in-time inventory, has left these systems vulnerable to unexpected shocks. As the Harvard Business Review points out:
"The search for supply chain efficiency has come at the cost of resilience, with hospitals and health care providers now dependent on fragile global supply chains vulnerable to disruptions from 'black swan' events like COVID-19." [2]
These vulnerabilities extend beyond cost-saving measures. Natural disasters - like hurricanes or wildfires - can damage medical equipment with heat and humidity, disrupt transportation routes, and cause power issues that affect device functionality [9]. On top of that, geopolitical conflicts and trade disputes can abruptly cut off access to critical components, while regulatory changes and opaque sourcing practices can expose hidden risks, often too late to address effectively.
One of the biggest challenges is the lack of reliable data and visibility. Over two-thirds of supply chain leaders report difficulties with accessing and integrating data [2]. This gap can lead to undetected shortages - where supplies exist but aren't visible - causing unnecessary spending on surplus stock while still facing localized shortages. Worse, misdiagnosing supply chain problems (e.g., attributing delays to warehouse capacity when the real issue is something as specific as packaging ink shortages) can lead to wasted resources and ineffective solutions.
Below, we explore how third-party vendor dependencies and cybersecurity threats add further layers of complexity to these challenges.
Third-Party Vendors and Supply Chain Reliability
Healthcare providers rely on a vast network of third-party vendors to supply everything from medical devices to administrative systems. Many organizations juggle over 1,200 agreements with group purchasing organizations (GPOs) and local vendors, each with complex pricing structures [5]. This setup creates a "concentration risk", where disruptions at a single vendor can ripple across the entire system.
Single-source dependencies make this problem even worse. Disruptions caused by geopolitical events, natural disasters, or operational failures can halt supply availability entirely. Providers are then forced to scramble for costly alternatives, pay for expedited shipping, or accept lower-quality substitutes [6] [7] [8]. When essential supplies like personal protective equipment (PPE) or life-saving drugs are unavailable, patient care suffers directly.
Fragmented communication between manufacturers, distributors, and healthcare providers only compounds these challenges. Poor interoperability can delay responses during critical moments [6]. To address these risks, many organizations are diversifying their supplier networks across regions and adopting "just-in-case" inventory strategies to prioritize stability over minimal stock levels [6] [8]. For example, Johnson & Johnson has committed over $5 billion to expand manufacturing within the U.S., reducing reliance on international production and mitigating trade-related risks [7].
While vendor-related risks threaten the physical flow of supplies, the increasing reliance on digital systems introduces new cybersecurity vulnerabilities.
Cybersecurity Threats to Patient Safety
As supply chains become more digitized, they also become more exposed to cybersecurity threats - risks that can directly impact patient safety. Sensitive patient data and supply chain information now move across interconnected platforms, creating opportunities for breaches that can disrupt operations. A single cyberattack can compromise patient records, disable medical devices, or halt critical supply chain functions.
Erik Decker, Vice President and CISO at Intermountain Health, highlights this systemic risk:
"The health sector's interconnected ecosystem means that a single vendor failure can cascade across critical functions and directly threaten patient care." [1]
Ransomware attacks are particularly dangerous, as they can bring entire systems to a standstill. When vendor platforms are compromised, hospitals lose access to essential tools like inventory tracking, ordering systems, and claims processing. These disruptions not only delay care but also risk non-compliance with regulations like FDA, HIPAA, and DSCSA, leading to legal and financial consequences [6] [7].
To counter these threats, many healthcare organizations are adopting secure, cloud-based platforms for supply chain management. By 2026, nearly 70% of U.S. hospitals and health systems are expected to transition to cloud-based solutions [5]. However, technology alone isn't enough. Building resilience also requires investing in staff training, fostering stronger supplier relationships, and ensuring that processes are in place to respond to cyber incidents effectively.
Identifying these risks is the first step toward creating a supply chain strategy that integrates both cybersecurity and vendor management.
| Risk Category | Specific Vulnerabilities | Impact on Care/Operations |
|---|---|---|
| Operational | Labor shortages, lean inventory, lack of alternatives | Procedure delays, expired products, manual workarounds |
| Environmental | Hurricanes, wildfires, heat/humidity, power outages | Contaminated devices, disrupted deliveries, equipment failures |
| Cyber/Systemic | Ransomware, vendor concentration, PHI breaches | System outages, compromised data, clinical downtime |
| Data/Technical | Poor data quality, lack of integration, invisible inventory | Forecasting errors, overspending, localized shortages |
Developing a Supply Chain Continuity Plan
Creating a strong continuity plan starts with identifying vulnerabilities before they become major problems. Misdiagnosing supply chain delays can waste resources and leave critical issues unaddressed. The goal is to pinpoint the root causes and focus efforts where they matter most.
Once you’ve identified the key issues, your plan should address three main areas: understanding which supply chain functions are essential for patient care, diversifying supplier relationships, and managing inventory to balance efficiency with readiness. This isn’t a one-time task - it requires continuous attention and adjustment.
Consider these statistics: nearly a quarter of hospital staff have seen recalled or expired products used on patients, and over half of clinicians recall instances where necessary supplies were unavailable for procedures [2]. A well-thought-out continuity plan can bridge these gaps.
While strong supplier relationships helped many organizations during recent disruptions - 50% of leaders noted these relationships reduced pandemic impacts [2] - relationships alone don’t suffice. Structured systems for risk assessment, backup sourcing, and inventory management are equally important. Let’s break this down further.
Business Impact Analysis (BIA) for Supply Chains
A Business Impact Analysis (BIA) helps identify which supply chain functions are critical and what happens if they fail. This isn’t about listing every product you purchase. Instead, it’s about understanding how third-party products and services connect to the 17 critical functions that keep healthcare running, like pharmacy operations, blood services, and claims processing [1].
The Health Sector Coordinating Council's (HSCC) Sector Mapping and Risk Toolkit (SMART) is an excellent resource. Developed with input from over 80 healthcare organizations, it maps how IT systems and third-party services tie into clinical and business operations [1]. The focus is on identifying "chokepoints" - those single points of failure where a disruption can ripple across multiple essential services.
To make BIA effective, prioritize resources based on real risks, not internal politics. Use a standardized scoring system (e.g., 300–850) to evaluate factors like protected health information (PHI) interaction, electronic health record (EHR) connectivity, and breach history [1]. This ensures you’re addressing the most critical vulnerabilities.
For essential products, calculate a "protection volume" - an optimal inventory level based on demand, lead times, and holding costs [10]. This gives you a clear safety stock target instead of relying on guesswork. Go beyond Tier 1 suppliers and map subtier suppliers to identify upstream risks, like raw material shortages, that could disrupt your operations [2].
Once you’ve mapped critical functions, move on to assessing and diversifying supplier risks.
Supplier Risk Assessments and Backup Sourcing
After completing a BIA, evaluate your suppliers to identify and mitigate vulnerabilities. Key factors to assess include financial stability, geographic location, cybersecurity, and regulatory compliance. The Centers for Medicare & Medicaid Services (CMS) requires Supply Chain Risk Management (SCRM) plans to be reviewed annually, setting a clear standard for reassessments [11].
Geographic diversification is a smart way to reduce risk. Partner with suppliers in different regions to avoid disruptions caused by natural disasters, geopolitical conflicts, or other localized issues [4]. Local sourcing for critical medical supplies can also help reduce reliance on complex international logistics and shorten lead times in emergencies [4].
Contracts should include clauses requiring vendors to notify you immediately of security breaches, software tampering, or unauthorized third-party involvement [11]. Ensure suppliers are vetted for compliance with federal regulations and don’t have ties to foreign entities that could pose security risks [11]. For medical devices, work with authorized distributors and require documentation to prevent counterfeit goods from entering your supply chain [11].
Regular audits of suppliers can help catch safety or regulatory issues before they escalate [4]. Staff training is also essential - equip employees to detect counterfeit products using industry-standard tools [11]. CMS’s two-person rule for validating component changes is another safeguard to consider for high-risk items [11].
Flexible contracts are key. Work with suppliers on agreements that allow for demand surges and require transparency about potential disruptions [4]. During COVID-19, organizations with strong supplier partnerships fared better than those with purely transactional relationships.
Once supplier risks are managed, focus on inventory strategies that balance efficiency with preparedness.
Inventory Management and Demand Forecasting
Traditional "just-in-time" (JIT) inventory models prioritize cost savings by keeping stock levels low. While efficient under normal conditions, this approach leaves organizations vulnerable during supply chain disruptions. A hybrid inventory model - combining JIT for routine items with "just-in-case" (JIC) stocks for critical supplies - offers a more resilient solution [4].
Identify which products need safety stock based on their importance to patient care, lead times, and susceptibility to disruptions. For these items, calculate buffer levels that account for demand variability and supplier reliability. Consider arrangements like Vendor-Managed Inventory (VMI) or Consignment Inventory (CI), which shift stock rotation and expiration management to suppliers with better forecasting expertise [10].
Modern demand forecasting tools use artificial intelligence and machine learning to analyze historical data, demographic trends, and health factors. These tools provide more accurate predictions than traditional methods, but they require clean, integrated data across your organization to work effectively [4].
Data quality remains a challenge - over two-thirds of supply chain leaders report issues with poor data and integration during disruptions [2]. Investing in supply chain "control towers" can provide real-time visibility of inventory across all locations, helping detect "hidden shortages" where supplies exist but aren’t accessible [2]. These platforms can prevent unnecessary spending on surplus stock while addressing localized shortages.
Technologies like IoT sensors, RFID tags, and GPS monitoring offer visibility into shipment locations and storage conditions for sensitive materials [4]. This is especially useful during disruptions when you need to redirect supplies quickly. Establish warehouses near healthcare facilities to reduce lead times in emergencies [4].
The shift to digital supply networks represents a broader evolution from linear supply chains to interconnected ecosystems. In 2021, 63% of healthcare organizations planned to increase technology investments, with 61% citing COVID-19 as the driving factor [2]. However, technology alone isn’t enough. Staff training is essential to ensure employees can leverage these tools for higher-value tasks instead of manual tracking [2]. The end goal is building a resilient system, not just deploying software.
Aligning Supply Chain Continuity with Cybersecurity Risk Management
In today’s interconnected world, supply chain disruptions and cybersecurity breaches are two sides of the same coin. Healthcare supply chains, heavily reliant on digital systems, are especially vulnerable. A single weak link - like a compromised third-party vendor - can send shockwaves across an entire network. For example, a cyberattack targeting one provider could jeopardize multiple hospital systems simultaneously. This "one-to-many" risk underscores the need for procurement and IT teams to work together to secure the supply chain.
The stakes couldn't be higher. In 2024, over 276 million individuals had their protected health data stolen or compromised due to breaches [14]. Healthcare also accounted for 16% of all ransomware attacks during the last quarter of 2023 [14]. These aren't just IT headaches - they can halt surgeries, delay critical treatments like chemotherapy, and disrupt prescription processing. As LevelBlue aptly puts it:
"Securing the healthcare supply chain is not just a technical task, but rather, it's a duty of care" [13].
Cyberattacks force IT and procurement teams to shift focus from patient care to crisis management. With nearly 80% of companies struggling to find and retain supply chain management talent [14], isolated efforts are no longer viable. Tools like Censinet RiskOps™ are emerging as essential bridges between procurement and IT risk management, offering a unified approach to tackling these intertwined challenges.
Using Censinet RiskOps™ for Supply Chain Risk Management
Censinet RiskOps™ simplifies the evaluation of supplier reliability and cybersecurity readiness by consolidating key assessments - like financial stability, geographic risks, and compliance - into one platform. This eliminates the need for juggling multiple tools, allowing teams to view all critical vendor data in one streamlined interface.
Automated workflows save time by replacing manual processes. For instance, with Censinet AITM™, vendors can complete security questionnaires almost instantly. The system automatically summarizes evidence and documentation, even identifying risks tied to fourth-party suppliers (vendors' vendors). Real-time dashboards provide a centralized view of risk, helping teams pinpoint which suppliers pose the greatest threat to essential functions like pharmacy operations or blood services. This collaborative risk network also enables organizations to share threat intelligence and best practices, cutting down on redundant efforts.
By integrating supply chain continuity planning with cybersecurity evaluations, healthcare organizations can proactively address vulnerabilities. If a vendor's cybersecurity measures are found lacking, procurement teams can demand improvements or activate contingency plans, such as backup suppliers, before a disruption occurs. This naturally promotes collaboration across departments, as explored below.
Cross-Department Collaboration for Risk Management
Managing supply chain risks effectively requires breaking down barriers between procurement, IT, and clinical teams. Each plays a vital role: procurement oversees supplier contracts, IT secures digital infrastructure, and clinical teams identify essential supplies. Without coordination, critical gaps can emerge, undermining even the most well-thought-out continuity plans.
Joint vendor risk management is a great starting point. Before onboarding a supplier, evaluate both their operational capabilities and security threats in their third-party relationships. Contracts should clearly outline vendor obligations, including breach notifications, data protection measures, and HIPAA compliance. As the Cloud Security Alliance emphasizes:
"Internal security policies of a HDO need to be upheld to include external supply chain risk and vendor assessments, as a compromised network can put systems at risk" [12].
Unified incident response protocols are equally essential. When disruptions or breaches occur, teams need clear, pre-established plans for containment and recovery. These should include defined roles, communication channels, and backup suppliers. Regular cross-departmental drills can expose weaknesses ahead of time, fostering smoother collaboration during real crises.
A security-first mindset should extend beyond IT departments. Regular training for frontline staff and administrators on phishing, multi-factor authentication, and password hygiene ensures internal defenses align with the standards expected of external vendors. As Zac Amos, Features Editor at ReHack, explains:
"For providers, protecting the supply chain is as critical as protecting the network" [14].
With the global average cost of a data breach projected to hit $4.4 million by 2025 [14], the value of cross-department collaboration cannot be overstated.
Diversifying sourcing is another key strategy for resilience. Relying on a single supplier for critical drugs or digital tools increases vulnerability. Procurement teams should work with IT to identify high-risk vendors - those handling sensitive data or central systems - and establish backup arrangements. This proactive approach reduces the impact of cyber incidents while maintaining operational flexibility.
Managing and Recovering from Supply Chain Disruptions
When supply chain disruptions hit, the stakes are high - patient care is directly on the line. Addressing these challenges takes more than quick fixes; it demands a coordinated and well-thought-out approach to protect operations and, ultimately, patient safety.
The first step in recovery is digging into the root cause. Is the disruption due to an actual shortage, or is it a result of poor inventory tracking? This distinction is critical because each scenario requires a different solution. For true shortages, the focus shifts to activating backup suppliers and repositioning inventory. On the other hand, visibility issues call for better tracking systems and stronger communication protocols to ensure clarity and accuracy in inventory management [2].
During active disruptions, conservation strategies become the lifeline. Adjustments like modifying surgical protocols to reduce disposable usage or safely reusing certain sterilized devices can stretch supplies without compromising care quality [3]. These measures buy time while alternative suppliers or logistics routes are secured. This approach lays the groundwork for implementing structured incident response protocols, which are essential for navigating crises effectively.
Resilient organizations rely on Memoranda of Understanding (MOUs) to establish emergency resource-sharing agreements and backup distribution plans [3]. They also maintain secondary distributor lists and identify alternative delivery locations to ensure supplies reach their destination, even when primary channels fail. For areas prone to natural disasters, pre-staging inventory ahead of predicted events like hurricanes can be a game-changer.
Incident Response Protocols for Supply Chain Disruptions
A structured response protocol can turn chaos into order. Frameworks like the Hospital Incident Command System (HICS) and the 10 Elements for a Continuity of Operations Plan (COOP) provide clear roles, responsibilities, and decision-making structures when every second counts [16].
Mapping critical functions is a key part of this process. Tools such as the HSCC SMART framework help align essential products and vendors with the 17 critical healthcare functions, such as pharmacy operations, diagnostic radiology, and claims processing [1]. This mapping allows teams to quickly identify vulnerabilities and activate contingency measures when disruptions occur.
Effective communication is another cornerstone. Beyond internal updates, organizations must coordinate with community partners, federal responders, and state agencies [15]. Establishing backup communication channels ensures that updates on shortages or delivery delays continue, even if primary systems like phones or the internet go down.
Clear escalation procedures are also essential. Teams need to know exactly when to activate backup suppliers, implement conservation measures, or notify regulatory agencies to keep operations running smoothly.
Testing Recovery Plans and Learning from Incidents
A recovery plan is only as good as its execution. Regular testing - through simulations, tabletop exercises, or full-scale drills - helps identify weaknesses before a real crisis hits. These drills validate coordination, technical systems, and recovery processes, ensuring that teams are ready when disruptions arise.
Routine audits of suppliers, warehouses, and distributors are equally important. These checks can uncover vulnerabilities long before they become serious issues [4]. With less than 10% of supply chain leaders rating their systems as highly resilient [2], there’s a clear need for continuous improvement.
Real-world events offer valuable lessons. For example, healthcare organizations refined their protocols after incidents like the Ebola outbreak and the Pulse Nightclub shooting, using those experiences to strengthen future supply chain risk responses [16]. Documenting these lessons and sharing them across departments builds a knowledge base that makes organizations better equipped for the next challenge.
Shifting from reactive to proactive management requires investment in tools like real-time tracking, AI-driven forecasting, and automated risk assessment platforms. These technologies not only enhance day-to-day operations but also provide a strong foundation for navigating future disruptions.
Updating and Improving Supply Chain Continuity Plans
In the fast-moving healthcare industry, keeping your supply chain continuity plan up to date is critical. New vendors, shifting regulations, and unexpected threats mean that treating your plan as a static document simply won’t cut it. Organizations that regularly revisit and refine their strategies are the ones that stay prepared for disruptions.
The problem is, many organizations still rely on outdated methods that don’t reflect today’s interconnected risks. A plan that worked a couple of years ago might now overlook key vulnerabilities in your vendor network or supply routes. Research highlights that many struggle to maintain resilient supply chains because they treat continuity planning as a one-and-done task rather than a continuous process.
To stay ahead, organizations need to monitor their vendor ecosystem and spot emerging threats. This requires investing in proactive tools and maintaining a mindset of constant improvement. As Deloitte aptly puts it:
"Supply chain resilience is a journey, not a destination" [2].
Tracking Emerging Risks and Industry Trends
Keeping your supply chain resilient means keeping an eye on a wide range of factors. Regulatory updates, geopolitical events, and industry-wide disruptions all have the potential to reveal weak spots in your supply chain, making systematic monitoring essential.
One effective approach is root cause analysis. For instance, during the COVID-19 pandemic, a manufacturing company discovered that its real bottleneck wasn’t raw materials but the ink used for printing expiration dates on packaging [2]. Digging deep like this ensures resources are directed toward solving the actual problem.
Another key strategy is mapping critical functions. The Health Sector Coordinating Council (HSCC), in collaboration with over 80 healthcare organizations, spent 16 months identifying 17 essential functions that support healthcare delivery, such as pharmacy operations and diagnostic radiology [1].
Building on this, in February 2026, Censinet launched a platform that operationalizes the HSCC SMART framework. It maps vendor products to these 17 critical functions, automatically visualizing dependencies and risks across entire portfolios [1]. Erik Decker, Vice President and CISO at Intermountain Health, explained the importance of this step:
"The challenge has always been operationalizing that insight - moving from understanding the risk conceptually to actually mapping, scoring, and managing it across thousands of vendor products." [1]
Establishing governance frameworks is another essential piece of the puzzle. Research shows that 80% of health system leaders see leadership as the main driver of digital transformation [2]. When supply chain leaders are part of strategic decision-making, continuity plans are better aligned with broader organizational goals.
Regular audits of suppliers, warehouses, and distributors can also uncover vulnerabilities before they lead to regulatory issues [4]. These audits aren’t just about compliance - they’re an opportunity to proactively address weaknesses.
Using Automation and AI for Supply Chain Continuity
Technology has become indispensable for managing modern supply chains. The sheer complexity of vendor networks and the speed at which threats emerge make manual tracking nearly impossible at scale. Platforms like Censinet RiskOps™ show how automation and AI can transform supply chain management.
AI-powered risk scoring changes the way organizations assess their vendors. Automated systems can assign FICO-like risk scores (ranging from 300 to 850) to vendor products, considering factors like PHI interaction, EHR connectivity, and breach history [1]. This helps prioritize which vendors pose the greatest risks to patient safety and operations.
Censinet’s RiskOps™ platform goes a step further, using AI research agents to evaluate risk factors automatically. It provides instant visibility into your risk portfolio without requiring manual assessments [1]. With data from over 200 healthcare organizations and 55,000+ vendors and products, the platform fills in gaps even when internal data is incomplete [1].
Demand forecasting tools powered by machine learning analyze historical data, demographics, and health trends to predict future needs [4]. This ensures inventory levels are adjusted in real time, preventing both shortages and overstocking. These algorithms continuously refine their predictions, adapting to seasonal and emerging patterns.
Real-time tracking using technologies like RFID, GPS, and blockchain offers visibility into shipments and warehouse conditions (e.g., temperature or humidity) [4]. Automated alerts can notify teams of delays or unacceptable conditions, enabling immediate action to protect products.
Predictive maintenance uses AI to schedule repairs for shipping fleets and warehouse equipment [4]. By anticipating issues before they occur, it helps prevent breakdowns that could disrupt the supply chain.
Shifting from reactive to proactive management takes effort, but the benefits are clear. As Ed Gaudet, CEO and Founder of Censinet, noted after the Change Healthcare attack:
"The Change Healthcare attack exposed what the industry has long feared but couldn't see: a single vendor failure can cascade across the entire health sector." [1]
With automated tools that map dependencies, score risks, and provide real-time insights, organizations can identify and address vulnerabilities before they escalate into larger problems that impact patient care.
Conclusion
Maintaining a steady and reliable supply chain in healthcare isn't a one-time effort - it’s a continuous process that requires strong leadership, smart investments, and a commitment to adapt over time. The numbers tell a concerning story: fewer than 10% of supply chain leaders view their systems as highly resilient, and 57% of hospital staff report situations where physicians lacked essential products during procedures [2]. These gaps pose serious risks to patient safety.
To address these challenges, healthcare systems need to move away from outdated just-in-time models and adopt Digital Supply Networks (DSNs). DSNs provide end-to-end visibility, enabling organizations to identify risks early and respond quickly to disruptions. But this shift isn’t just about technology - it requires a top-to-bottom commitment, with supply chain leaders playing an active role in strategic decisions [2]. The key lies in blending traditional approaches with modern digital tools.
One such tool is Censinet RiskOps™, which enhances risk management by mapping vendor products to 17 critical healthcare functions and using AI-driven risk scores to create a continuous, intelligence-based approach to managing risks [1].
However, technology alone isn’t enough. Effective governance and leadership are critical to this transformation. Organizations that combine tech investments with changes in processes and people - not just stockpiling supplies - are the ones that build true resilience. This involves digging into root causes to uncover vulnerabilities, setting up strong governance structures, and prioritizing visibility throughout the supply chain.
Building a resilient supply chain is an ongoing process [2]. By treating continuity planning as a proactive strategy and leveraging automation, robust governance, and strong supplier relationships, healthcare organizations can ensure uninterrupted patient care - even when disruptions are unavoidable.
FAQs
How do I decide which supplies need just-in-case stock?
To figure out which supplies need to be kept in just-in-case stock, look at how critical they are, how shortages could affect patient care, and any supply chain risks. Focus on items that are absolutely necessary for operations during emergencies - especially if they come from suppliers known to be unreliable or have long delivery times. Supplies that are difficult to replace or essential for patient safety should also be stocked to minimize risks during unexpected disruptions.
What should a supply chain Business Impact Analysis include?
A healthcare supply chain Business Impact Analysis (BIA) focuses on evaluating critical operations and understanding how disruptions could affect them. This involves pinpointing key vendors, recognizing supply chain dependencies, and identifying essential processes that directly influence patient care and overall system stability.
The BIA should thoroughly assess risks, such as cyberattacks or natural disasters, and establish contingency plans alongside clear recovery strategies. These measures are crucial for maintaining uninterrupted care, ensuring patient safety, and supporting operational stability. Regular testing and updates to these protocols are essential to keep the system prepared for potential challenges.
How can we reduce cyber risk from third-party vendors?
Reducing cyber risks from third-party vendors in healthcare requires a proactive and ongoing approach. This involves continuous monitoring, comprehensive risk assessments, and establishing clear contractual obligations.
Some key strategies include:
- Real-time vendor risk monitoring: Keeping a close eye on vendors' security practices to quickly identify potential vulnerabilities.
- Prioritizing critical vendors: Focusing efforts on vendors that handle the most sensitive data or provide essential services.
- Enforcing strict security standards in contracts: Clearly outlining security expectations and compliance requirements in vendor agreements.
Tools like Censinet RiskOps™ simplify these tasks by automating risk assessments and providing continuous oversight. Additionally, regularly testing incident response plans ensures healthcare organizations can act swiftly during breaches, protecting sensitive patient information and maintaining operational stability.


